Sorry, there are no results for . Please make another selection above or see below for more Gillette Stories.
Gillette Stories
Gillette Stories
At Gillette Children's we help every child in our care live a life defined by dreams, not diagnosis. Here you will find stories of inspiration and triumph and joy. Learn more about our work with patients and families that don't give up as we help every child live their story. Gillette Stories Magazine


Philanthropy
Meet Gillette Children’s Jessie’s Club Ambassador Adelynn McCoy
March 25, 2025Adelynn McCoy with KS95 Morning Show hosts at the 2024 KS95 for Kids Radiothon benefitting Gillette Children's and the M Health Fairview Masonic Children's Hospital Cancer Program.
Read More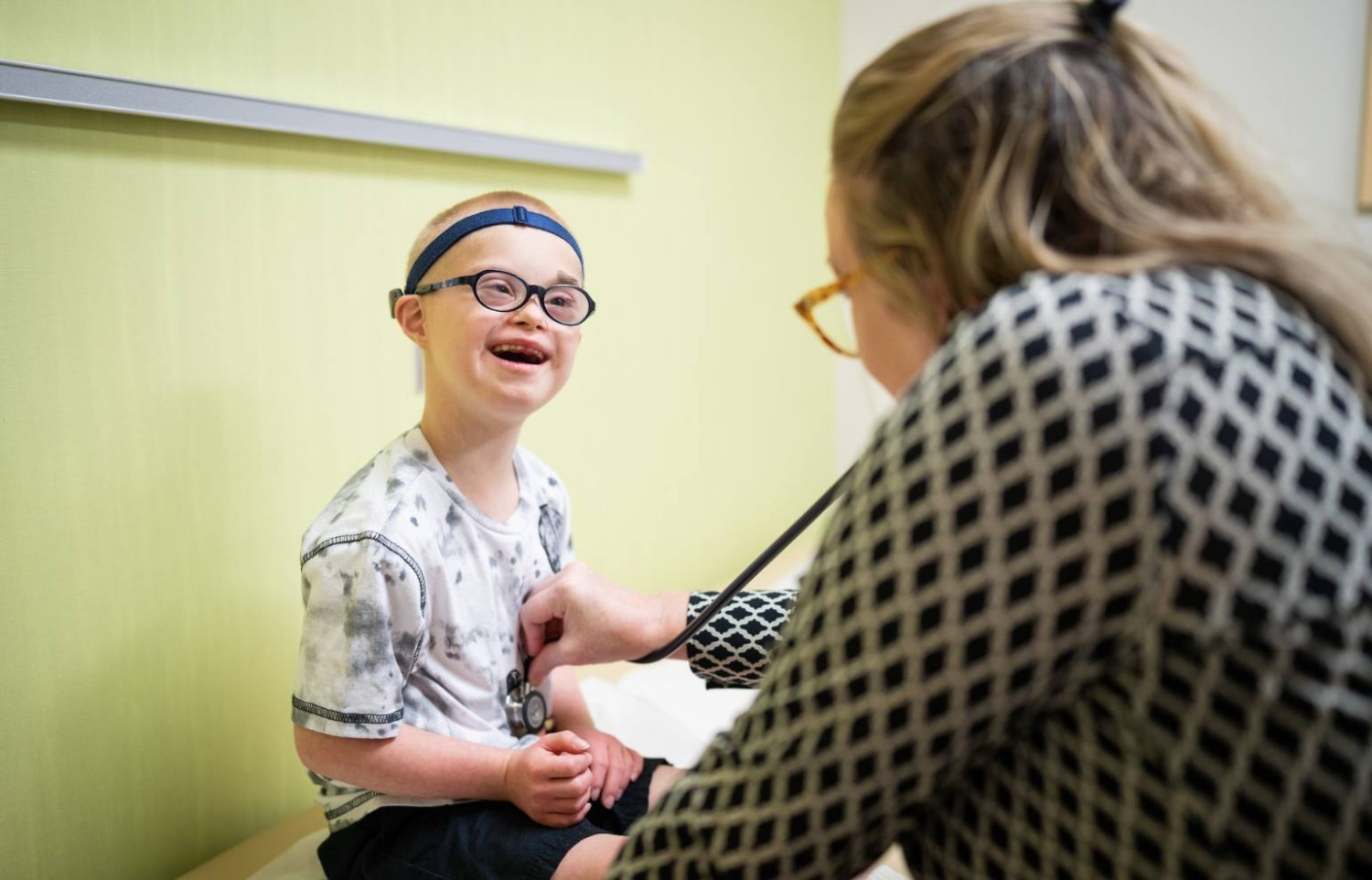
Featured Post
Down Syndrome and Healthcare: Your Questions, Answered
March 20, 2025Get answers to common questions about the kind of medical care that children with Down syndrome often need.
Read More
Innovation and Research
Gait and Motion Analysis Makes Gillette a Top Center for Cerebral Palsy Care
March 20, 2025The “gait lab” has helped thousands of people who have CP reach their full potential when it comes to walking and movement.
Read More
Innovation and Research
Transforming Outcomes for Hemiplegic Cerebral Palsy
March 15, 2025Gillette Children's study examines the use of Infant Constraint Induced Movement Therapy to improve outcomes for children with hemiplegic cerebral palsy.
Read More
Cerebral Palsy
Expanding Cerebral Palsy Knowledge with Three New Books
March 11, 2025With more than a century of unwavering commitment and expertise in cerebral palsy care, Gillette Children’s—through our Cerebral Palsy Institute—is a global leader in clinical excellence, pioneering research, and advocacy. In December 2024, we reached a new milestone with the release of three books as part of the Gillette Children's Healthcare Series, each focusing on a different type of cerebral palsy: Spastic Hemiplegia, Spastic Quadriplegia, Spastic Diplegia, second edition
Read More
Our Team
Developmental Evaluation Clinic Provides a Powerful Team of Experts
March 7, 2025Gillette Children’s has a new Developmental Evaluation Clinic to help answer parents’ questions about their child’s growth and development.
Read More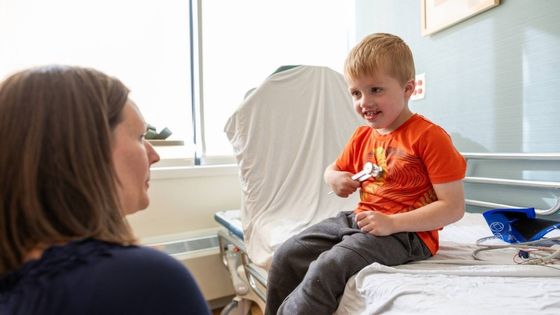
Rare Disease
Gillette’s Global Partnership Advances Care for Rare Disease
March 3, 2025Over 400 million people worldwide are estimated to live with a rare disease, and over half of those living with a rare disease are children. Gillette Children's has partnered with the International Hospital Federation (IHF) to form the Global Rare Paediatric Disease Network (GRPDN), a groundbreaking initiative aimed at improving care for children with rare diseases worldwide.
Read More
Rare Disease
What is Pediatric Genetic Counseling at Gillette Children’s
March 3, 2025Gillette Children’s is expanding its team of expert genetic counselors to help you find answers and make informed decisions about genetic testing and discover how a rare genetic disease might affect your child. Gillette provides solid information and support.
Read More
Philanthropy
Gillette Children’s Announces 2025 Children’s Miracle Network National Champion
March 3, 2025ZaLayaa Jahzara Wandrick is 12 years old. She’s an excellent cook, crafter and loves science, soccer and coding, but for much of her life, has had to deal with multiple sensory and complex medical conditions. Gillette Children's is excited to announce ZaLayaa Jahzara has been named our 2025 Children's Miracle Network National Champion.
Read MoreHealth Library
Find education related to your condition, procedure, care at home, and more.
Search Health LibraryResearch
Gillette Research aims to improve treatment options for children who have disabilities.
Explore Gillette ResearchNews
From innovations to innovators, Gillette Children’s shares our news as leaders in specialty care and research.
News Releases Home Page
Home Page
