Gillette Stories
Gillette Stories
At Gillette Children's we help every child in our care live a life defined by dreams, not diagnosis. Here you will find stories of inspiration and triumph and joy. Learn more about our work with patients and families that don't give up as we help every child live their story. Gillette Stories Magazine


Patient Stories
Leo St. Martin to Lead the Way in Gillette Children’s 2025 Walk & Roll Event
Leo St. Martin is Gillette Children's 2025 Children's Miracle Network Champion and 2025 Walk & Roll patient ambassador. He is all about sports. Baseball, football, hockey, soccer – you name it, he wants to play it. When he was an infant, Leo was diagnosed with Infantile Pompe disease, a rare genetic disease that leads to weakened muscles. His physical and occupational therapists helped get him into a power chair when he was just three, and they continue working with him, motivating him to make the impossible, possible.
Read More
Philanthropy
Rett Syndrome Research at Gillette Children’s Shows Promise
Generous support from donors has fueled advancements in Rett Syndrome research at Gillette Childrens.
Read More
Philanthropy
Leading the Gillette Children’s Philanthropy Board
Scott Ward, chair of the newly formed Gillette Children's Philanthropy Board.
Read More
Philanthropy
How the Nowicki Family is Giving Back After Their Son’s Recovery
The Nowacki family, inspired to give back to Gillette Children's by their son's care, gathers at Gillette's annual Walk & Roll community event.
Read More
Philanthropy
Family Engagement in Research: Real Lives, Real Impact
Gillette Children's Family Engagement in Research Coordinator, Haley Brunelle (left), draws on her experience as a caregiver to her son, Felix (center), in her work.
Read More
Our Team
What Makes Gillette Children’s Down Syndrome Clinic Unique?
Gillette Children’s Down Syndrome Clinic helps children and families navigate the health challenges that often come with this condition.
Read More
Innovation and Research
Palliative Care: What Parents and Caregivers Need to Know
Palliative care is focused on treating the pain and stress that a serious illness can cause. Read on.
Read More
Our Team
After Dark: Shining a Light on Evening and Night Shift Staff
An hour-by-hour look at the vital work performed by second and third shift employees at the St. Paul Campus.
Read More
Philanthropy
A Patient Journey Comes Full Circle
Former patient Elizabeth Lilley returned to Gillette 20 years later as a volunteer with Dairy Queen.
Read More
Philanthropy
Meet Jessie’s Club Ambassador Carter Mulvey
Through expert care from his Gillette Children's care team, support from his family, and a lot of determination, Carter has made huge strides with his mobility.
Read More
Philanthropy
Meet Gillette Children’s Jessie’s Club Ambassador Adelynn McCoy
Adelynn McCoy with KS95 Morning Show hosts at the 2024 KS95 for Kids Radiothon benefitting Gillette Children's and the M Health Fairview Masonic Children's Hospital Cancer Program.
Read More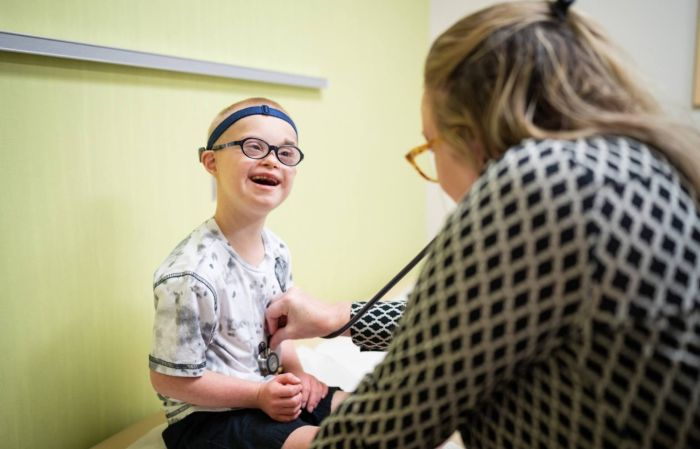
Featured Post
Down Syndrome and Healthcare: Your Questions, Answered
Get answers to common questions about the kind of medical care that children with Down syndrome often need.
Read MoreHealth Library
Find education related to your condition, procedure, care at home, and more.
Search Health LibraryResearch
Gillette Research aims to improve treatment options for children who have disabilities.
Explore Gillette ResearchNews
From innovations to innovators, Gillette Children’s shares our news as leaders in specialty care and research.
News Releases Home Page
Home Page
