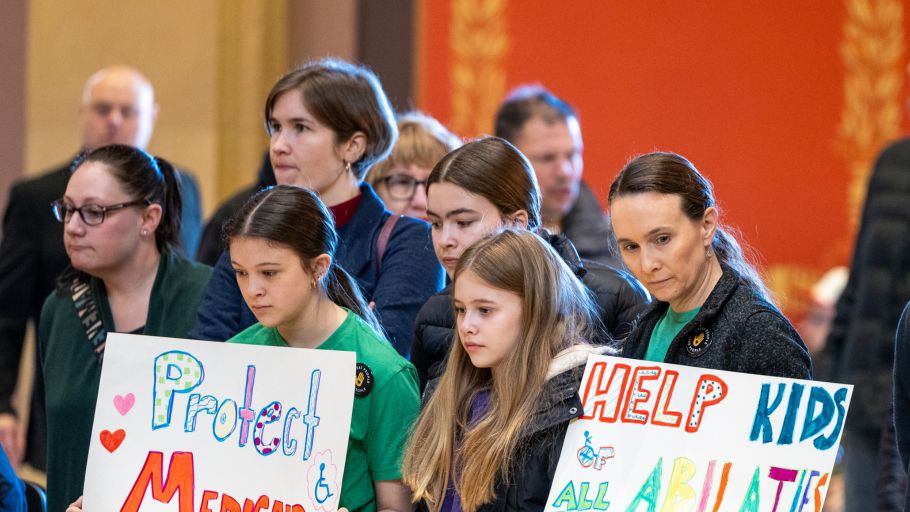A History of Advocacy at Gillette Children's
Gillette Children’s is founded on advocacy over 125 years ago. Before our first patient was served, Jessie Haskins led a pioneering effort to ensure that children with disabilities had a place to receive care. Jessie brought forward an issue to those who could legislatively create change and improve child wellbeing. She was introduced to Dr. Arthur Gillette, who knew she was a powerful ally. They partnered to lobby the Minnesota legislature to establish Gillette Children’s. Our legacy of advocacy for our patients lives on to this day.
Gillette Children's Advocacy Today
Today’s advocacy work at Gillette is done by patients, parents, staff, community members and elected officials. Together, we push for changes that improve the lives of Gillette patients and community members living with rare diseases and/or disabilities. We work with individuals, families and coalitions to identify and eliminate health inequities and disparities.
 Home Page
Home Page