Following your urology procedure, the doctor will insert one or more catheters (tubes) into your bladder to keep it empty of urine and allow it to heal:
- Foley catheter: a catheter inserted through your urethra (the place where you normally urinate) into the opening of your bladder.
- Suprapubic catheter: a catheter inserted into the top of your bladder through your lower abdomen.
- Mitrofanoff catheter: a catheter inserted into your bladder through your belly button. (Note: This catheter is clamped until the Mitrofanoff is ready to use.)
- ACE catheter: a catheter inserted into the lower part of your abdomen following an antegrade continence enema (ACE) procedure. (Note: This catheter is clamped until we teach you how use it.)
Urine draining from the bladder will be red or pink. This is part of normal healing and is nothing to worry about.
Other tubes and machines also will be in place following your procedure:
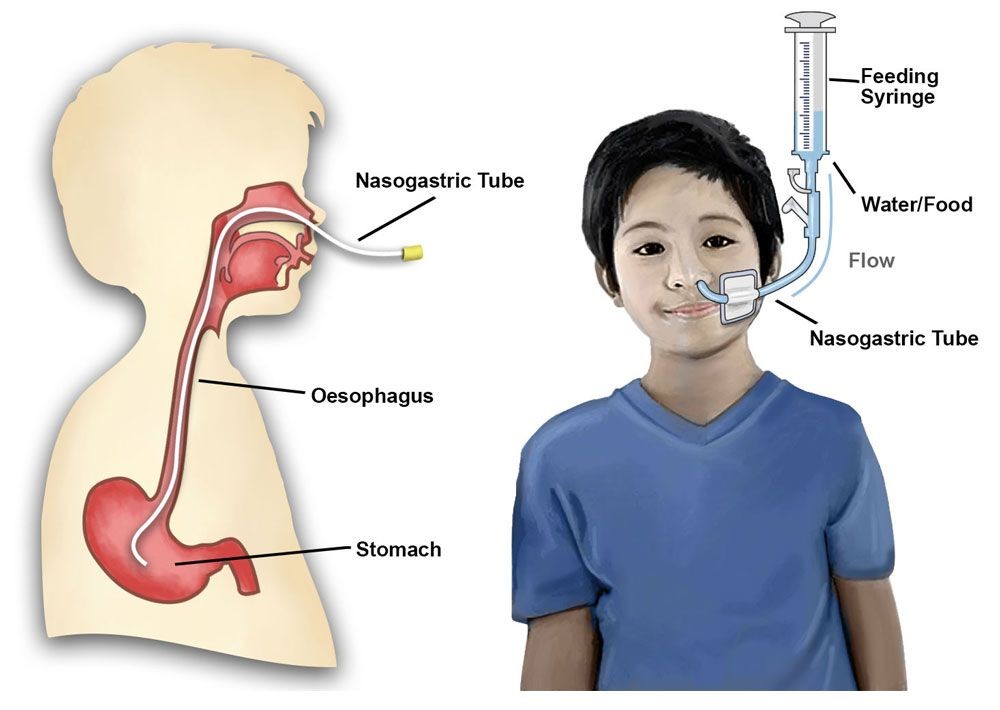
- Nasogastric tube (NG): a tube inserted through the nose and into the stomach to keep it empty until your bowel starts working again. The average time the tube stays in is 3-5 days.
- Cardio Respiratory (CR) Monitor: a machine that monitors your heart rate and breathing while you’re receiving pain medicine. Sometimes the monitor will alarm (beep). If this happens, don’t worry; the nursing staff will attend to the beep.
Comfort After Urology Surgery
Your doctor will decide which pain medicines are right for you. You may have an epidural or a patient controlled analgesia pump (PCA). Your nurse will give your pain medicine and fluids through your intravenous line (IV). Once you’re eating and drinking, you’ll take your medicine by mouth. We want you to be comfortable, so tell your nurse if you experience pain.
Nutrition and Fluids After Urology Surgery
After surgery, you won’t be able to eat or drink anything by mouth for a few days. You’ll have one or more IVs to provide the fluids, pain medicines and antibiotics needed to help you get better. When your bowel starts working again, the NG tube will be clamped or removed. Then you’ll gradually add foods to your diet, starting with clear liquids, such as juice and Jell-O. It’s important to drink plenty of fluids and eat a nutritious diet to help with your healing.
Activity After Urology Surgery
We encourage quiet activity for the first few days after surgery. When you’re ready, your nurse will help you get out of bed. Activity will keep your body strong while you heal. It also will help your bowel start working again.
Breathing Exercises
It’s important to take deep breaths and do breathing exercises while you recover so that you don’t get pneumonia. You might be given something called an incentive spirometer or bubbles to blow to help exercise and expand your lungs. The spirometer is a lung exerciser
that shows the amount of air you can inhale. Coughing is another exercise that you may need to do. If coughing is uncomfortable, you can place a pillow over your abdomen to ease discomfort.
Incision Care After Urology Surgery
Your incisions may be covered with a cloth dressing. These dressings will be changed or removed as needed. Some of your incisions will have stitches. Some of these stitches are simply used to hold the tubes in place as you heal and will be removed when you return to clinic for your follow-up appointment.
Learning Opportunities After Urology Surgery
Before you go home, we’ll teach you everything you need to know about how to take care of yourself at home. We’ll teach you how to irrigate your bladder, check for signs of infection and empty your urine bag. If you had an ACE procedure, we’ll show you how to use your ACE catheter. You’ll practice these skills before you go home. We’ll also give you supplies to get you started.
Discharge from the Hospital After Urology Surgery
You’ll be discharged when you’re eating and drinking well, you feel comfortable, you have no fever, and your bowel function has returned. When you go home, some of the catheters will still be in place. Some will be clamped, others will drain into a bag.
Follow-Up Appointments After Urology Surgery
About three weeks after surgery, you’ll return to the clinic for a follow-up visit. This is a good time to ask any new questions that you might have. You will have a test called a cystogram, which is an X-ray used to check the progress of your healing.
This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.
If you are a Gillette patient with urgent questions or concerns, please contact the Nurse Help Line at 651-229-3890.
 Home Page
Home Page
