What is bladder augmentation?
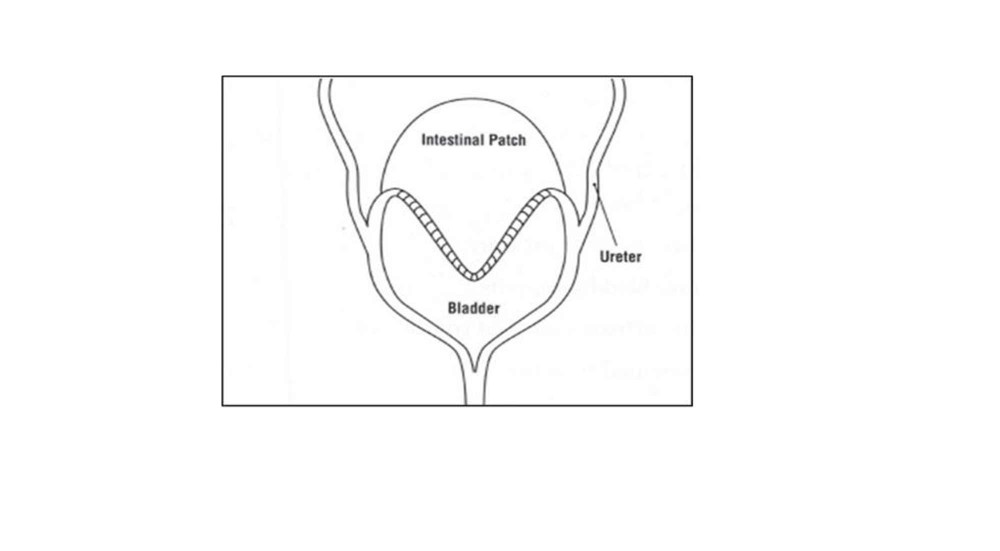
Bladder augmentation is a surgical procedure to enlarge the bladder so it can hold more urine at low pressure. This surgery is performed to prevent kidney damage from occurring. Bladder augmentation is often done for patients with a neurogenic bladder. Surgeons usually use pieces of intestine or stomach tissue to enlarge the bladder. After a bladder augmentation, the bladder needs to be emptied by catheterization throughout the day on a regular schedule.
Who benefits from bladder augmentation?
At Gillette Children's, bladder augmentation is performed most often on patients with a neurogenic bladder, which causes poor bladder control.
Neurogenic bladder may cause the bladder wall to become too stiff and unable to stretch when filling. When this happens, the pressure in the bladder gets too high and can cause kidney damage and urine leakage.
The success of a bladder augmentation procedure depends on careful patient selection. Good candidates for a bladder augmentation procedure are those who are physically capable and emotionally ready to handle a strict routine of intermittent catheterization and daily bladder irrigation. Another good candidate is someone whose caregivers are motivated, available, and trained to follow the catheterization and irrigation routine.
What should I expect with bladder augmentation surgery?
Below is a guide for what to expect before, during, and after bladder augmentation surgery.
After a day or two of home bowel preparation, you may be admitted to the hospital the day before surgery to continue cleaning your bowel. Cleaning out your bowel before bladder surgery helps reduce the risk of infections and complications. A nasogastric (NG) tube will be placed through your nose and into your stomach. The tube is used to give medicine that will clean out your intestine.
Blood tests are done on the day of admission. An intravenous (IV) tube may be started to ensure you get enough fluids. Antibiotics may be given through your IV as well. You will receive specific instructions on what you may eat or drink before surgery.
Bladder augmentation surgery may last many hours.
Following surgery, one or more catheters may be in place to keep the bladder empty and allow it to heal:
- Foley catheter: a tube that’s inserted through the urethra (the place where you usually urinate) into the opening of the bottom of the bladder.
- Suprapubic catheter: a tube inserted into the bladder through the lower abdomen.
- If you have a continent catheterizable channel created as part of your surgery (such as during a Mitrofanoff procedure), you will also have a catheter inserted to keep the new channel from closing.
A catheter will continuously drain urine from your bladder for at least three weeks after surgery. Please note that your urine may be red or pink with some blood clots and mucus.
You'll have an IV to give you medicine, fluids, and nutrition. Your incision will be covered.
After surgery, you won’t be able to eat or drink anything by mouth. Within a few days, when bowel activity resumes, the NG tube will be removed, and your diet will advance slowly from clear liquids to full liquids to soft foods. This transition usually takes anywhere from three days to a week. You’ll need to drink plenty of fluids. A nutritious diet promotes healing.
You’ll be discharged when you can tolerate a regular diet, use oral pain medicines, have no fever, and have resumed regular activity.
Bladder Augmentation Recovery
One or two catheters may be in place when you leave the hospital. One may be clamped off, with the other draining into a drainage bag. Check the drainage bag to make sure urine is collecting into the bag, and none of the tubing is kinked. You will learn how to flush the catheter if urine stops flowing or if urine leaks around the catheter. If you use a Foley catheter, you must secure the catheter tubing to your leg to prevent the catheter from pulling on and irritating your urethra. Clean around the catheter(s) daily with soap and water and pat dry. You should empty the drainage bag(s) at least twice daily.
See below for further instructions on recovering from bladder augmentation surgery at home.
You will receive instructions on caring for your abdominal dressing before leaving the hospital. Watch for signs and symptoms of infection:
- Increased pain
- Increased body temperature
- Swelling at the incision site
- Draining from the incision site
- Redness at the incision site
- Change in the smell of urine
Call your surgeon's office immediately if you notice any of these symptoms.
Do not soak or swim in a lake, pool, or hot tub (as directed by your surgeon).
It's essential to drink plenty of water every day. Adequate fiber intake can help reduce constipation. Practice a regular bowel program to avoid chronic constipation.
You may return to school or work when you feel well enough to do so or when your surgeon says it's OK. You shouldn't participate in swimming, wrestling, riding bikes, or other strenuous activities for at least three weeks after surgery or until your catheters are removed.
The tissue used to create your bladder augmentation will continue to secrete mucus. To help prevent mucus build-up, irrigate (flush out) your bladder with normal saline at least twice daily for the first two to three months following surgery. After that, irrigate the bladder at least once daily for the rest of your life. Please see bladder irrigation for more information.
Post-Operative Follow-Up
About two or three weeks after discharge, you'll have a test called a cystogram. In a cystogram, contrast (colored) fluid will be put into the bladder via a catheter. If all of the contrast fluid stays in your bladder and there are no leaks, then one or all catheters may be removed by your surgeon. After the catheters are removed, you will start intermittent catheterization to drain your bladder. A urology provider will teach you how to irrigate your bladder to prevent mucus buildup, bladder stones, and urinary tract infections (UTIs).
Medical Identification
It is essential that you wear some form of medical identification indicating that you have an augmented bladder in case of an emergency. If you had a Mitrofanoff procedure, your identification should state that you must be catheterized through the Mitrofanoff site.
When to Call Your Gillette Provider
Call your Gillette surgeon if:
- your urine output decreases and does not improve after irrigating your catheter(s)
- your catheter(s) fall out
- you are unable to irrigate your catheter
- there is a large amount of bleeding
- you notice signs or symptoms of an infection (the incision is red, swollen, draining, or if you have a fever of 101.5o F or higher).
For More Information
If you have health-related questions on this topic, please call the Gillette Nurse Help Line at (651) 229-3839.
This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.
If you are a Gillette patient with urgent questions or concerns, please contact the Nurse Help Line at 651-229-3890.
 Home Page
Home Page
