What is a Gastrostomy Tube (G-Tube)
Gastrostomy tubes are soft, flexible tubes, which are placed in the stomach and used for feeding individuals who have difficulty eating.
The gastrostomy tube is inserted during surgery. A small hole called a “stoma” or “gastrostomy” is made in the abdomen. The tube usually remains in the stoma. If the tube is removed, the stoma may get smaller and even close.
Gastrostomy tubes may be used full-time with no oral feedings, or part-time as a feeding supplement for liquids or during illness. Your doctor will let you know what can be eaten orally and what should be given through the tube.
Caring for gastrostomy tubes is simple. Your nurse or doctor can teach you how to change the tubes at home. Remember to take notes so you can reference them later.
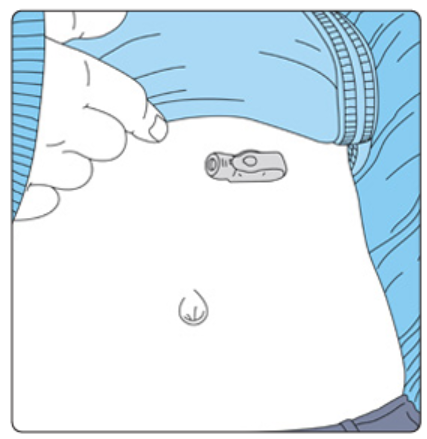
Illustrates where G-Tube is placed.
Why would my child need a gastrostomy tube?
Children with developmental disabilities, such as cerebral palsy, are at risk for different feeding problems. The decision to place a gastrostomy feeding tube is often difficult for families. \It is important for families to realize that the reason their child needs a feeding tube is related to the child’s disability and does not reflect the family’s efforts.
- Poor growth (despite dietary supplements). A child who grows poorly may become chronically undernourished. This places a child at risk for many problems including: increased risk of infections, poor wound healing after surgery, poor healing of skin sores and overall decreased energy with less potential for development.
- Significant time and effort involved with feedings. Many patients with underlying neuromuscular diseases have difficulty swallowing, which can frustrate families. The increased time required for feedings may decrease the time you and your child have for other activities.
- Aspiration. Aspiration occurs when contents from the mouth or stomach go into the breathing tube or lungs during oral feedings, resulting in recurrent respiratory problems (infections, wheezing, etc.). Aspiration may cause discomfort, decreasing your child’s interest in feeding.
After tube placement, your child will be in the hospital for approximately 1-2 days to develop the best tube feeding schedule for you and your child, and to be sure your child is tolerating the feedings prior to discharge. You will be given instructions about using and caring for the tube before your child leaves the hospital. You will also be given the phone number of a clinic nurse to call if you have questions or problems after you go home.
Some children will regain the ability to meet their nutritional needs by mouth. In this situation, a gastrostomy tube can be removed and the site will then heal over.

Children who do not aspirate are often able to continue eating by mouth after the feeding tube is placed. Oral intake may be more pleasant when there is no stress or pressure associated with having to feed enough for all the child’s needs. Your doctor will let you know if your child can still eat by mouth or receive oral stimulation. (An oral stimulation handout is available). Your doctor will tell you what formula should be given through the tube
It may be helpful for you to talk with a family who has a child with a gastrostomy feeding tube and hear about their experience. Please let us know if you would like to do this. In addition, we are available for any questions you may have. Please let us know how we may assist you in this decision.
Translations
Video Resources
View Gastrostomy Tube Care Videos at gillette.mn/G-Tube or scan QR Code.

This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.
If you are a Gillette patient with urgent questions or concerns, please contact the Nurse Help Line at 651-229-3890.
 Home Page
Home Page
