Some children need a tracheostomy (trach) tube to help them breathe with a clear airway. They might depend on a trach tube temporarily or they might rely on it over their lifetime. Either way, parents and caretakers need to practice good habits when changing and
What is an emergency trach kit?
An emergency trach kit contains everything you need to help your child breathe again if the trach tube comes out accidentally or becomes blocked. Before your child comes home from the hospital, gather what you need for your emergency trach kit. Then keep the kit with your child at all times, whether your child is at home, at school, visiting friends or elsewhere.
What should I keep in an emergency trach kit?
Always have these items in your child’s emergency trach kit:
- Two clean trach tubes with holders attached and obturators in place:
- One tube that’s the same size as the tube your child has in place
- One tube that’s a size smaller than the tube your child has in place
- Trach ties (twill tape, Velcro or bead chain)
- Trach noses
- Spare inner cannula (if needed)
- Small blanket or towel roll
- Blanket for mummy restraint (if needed)
- Sterile water
- Water soluble lubricant
- Saline lavage (if used at home)
- Suction and catheter kits
- Portable suction machine
- Bulb syringe — for one-time shallow suctioning if no power is available
- Manual resuscitation bag and face mask
- Luer-Lock syringe (if trach tube is cuffed)
- Instructions for cardiopulmonary resuscitation (CPR) and troubleshooting an obstructed tube
- Bandage scissors
- Tissues
- Tweezers or forceps
- Wipes or hand sanitizer
- Oxygen tank
- Emergency phone numbers
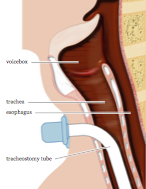
What should I know before I change the trach tube?
Typically, a trach tube requires changing every one to four weeks to prevent mucus buildup and to keep it clean. However, this frequency might vary depending on your child’s needs and what your doctor advises.
Trach tube changes should happen before feeding or at least two hours after feeding.
Always change the trach tube with two people present — unless it’s an emergency and this isn’t possible.
Before changing a trach tube, you need to know some basic information. You should be able to answer the following questions correctly and confidently.
- Is this a new tracheostomy or an established one?
- Is the trach tube cuffed or uncuffed?
- Is there an inner cannula?
- Can your child breathe on his or her own, or is he or she dependent on a ventilator?
- Do you have suction set up and ready to use?
- Where are your backup trach tubes, trach ties, syringe and lubrication?
- Do you know how to use a manual resuscitator?
If you’re uncertain about your responses to any of the above questions, or if you have any questions about changing your child’s trach tube, talk to your doctor before starting the change process.
Once you’re confident in your knowledge about changing your child’s trach tube, you can begin.
How do I change a trach tube?
First, gather your supplies (included in the emergency trach kit).
Talk to your child, whether you’re making a routine change or changing a trach tube that’s fallen out by accident. Explain what you’re doing in a way that’s appropriate for your child’s age and understanding. Use a calm, gentle approach. Your child might sense this and become anxious if you appear anxious.
Follow these instructions:
- Wash your hands.
- Cut trach ties to the appropriate length.
- Inspect all tubes for cracks, tears, or decreased flexibility before you use them, especially if they are being reused. For cuffed tubes, inflate the cuff to confirm it’s functioning properly and check for leaks. Then, deflate the cuff completely before inserting the tube.
- Bring a trach tie through one end of the new trach tube. Avoid touching the part of the tube that is inserted into the trachea. Try to keep it sterile.
- Insert the obturator into the new tube. Be sure it slides in and out easily. The obturator helps guide the tube, and the rounded tip protects the stoma during insertion.
- Place a small amount of sterile water or soluble lubricant (Surgilube or KY Jelly) on the end of the new trach tube, and place the tube on a sterile tray or a clean surface until you’re ready to insert it. Note: Never use Vaseline or any petroleum jelly as a lubricant. If you use a lubricant, use it sparingly and wipe off any excess.
- Keep a suction machine, a catheter, and an oxygen tank handy in case they are needed.
- Place your child on their back with a small blanket or towel roll under the shoulders to help with slight hyperextension. It might be helpful to wrap your child in a blanket, mummy-style, especially if your child isn’t cooperative. Your child may also sit up for the trach tube change.
- Administer oxygen if directed by your doctor’s instructions.
- If your child has a cuffed trach tube, deflate the cuff and gently remove the old tube. (Follow the tube's angle, an upward and outward arc.)
- Release the old trach ties while holding onto the trach tube. Always hold the tube when ties aren’t secure; a cough can dislodge the tube.
- Insert the new tube in a smooth curving motion, directing the tip toward the back of the neck in a downward and inward arc (like inserting a suction catheter).
- Do not force the tube.
- Remove the obturator immediately while holding the tube securely with your other hand. Remember: Your child cannot breathe with the obturator in place.
- Changing the trach tube will cause your child to cough; do not let go of the tube.
- If the trach tube is a cuffed tube, inflate the cuff with the prescribed amount of air.
- Thread the trach tie through the other end of the tube and tie it, allowing one finger between the neck and the ties. You might need tweezers or hemostats to thread ties through the hole of the wing of the trach tube.
- Inspect the old tube for color, mucus plugs, or odor, and then set it aside. When changing a trach tube, look for skin irritation or breakdown and signs of infection.
- Remember to encourage and praise your child. A trach tube change can be emotionally difficult for some children.
What should I do if the track tube is blocked?
A blocked trach tube is an emergency: Your child cannot breathe. Help clear your child’s airway by following these instructions:
- Try suctioning through the trach tube.
- If the catheter doesn’t pass, change the trach tube. (See instructions provided earlier in this handout.)
- If you’re unable to proceed quickly, remove the trach tube, hold gauze over the stoma, and use the manual resuscitator to ventilate through your child’s mouth and nose.
- Change the trach tube when you’re ready.
When should I call the doctor?
Call your Gillette doctor if you notice any of the following:
- Redness, skin breakdown, or rashes around the stoma
- Fever: temperature above 101.5 F orally or 100.5 F under the armpit
- Signs of dehydration (getting dried out), such as:
- No urine (or wet diaper) for eight hours
- Urine color darker than normal
- Urine’s smell stronger than normal
- Mucus is yellow, green, red, or blood-tinged, or it develops a smell
- Any breathing problem that doesn’t get better after suctioning
Call 911 if:
- Your child is bleeding more than a little from the trach tube. Do not remove the trach tube; suction it often until trained help takes over.
- Your child stops breathing.
- Your child becomes unconscious.
- You feel you cannot handle the situation.
- You have to do CPR.
- You have to do an emergency trach tube change and are concerned about it.
This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.
If you are a Gillette patient with urgent questions or concerns, please contact the Nurse Help Line at 651-229-3890.
 Home Page
Home Page
