What Is Upper Extremity Functional and Intensive Therapy (UFIT)?
Gillette’s upper extremity functional and intensive therapy (UFIT) program includes a variety of treatments and techniques to help patients build strength, coordination, and range of motion in their arms and hands. UFIT uses upper extremity movements—initiated by the patients—to help them improve their ability to use their arms in functional tasks.
We might recommend UFIT using the ArmeoSpring for patients who have weakness in one or both arms, including people who have one of the following conditions:
- Brachial plexus injuries.
- Cerebral palsy.
- Traumatic brain injuries.
- Stroke.
- Spinal cord injuries and related neurotrauma.
- Neuromuscular conditions.
- Spasticity and increased muscle tone in the upper extremities.
What Is ArmeoSpring Therapy?
ArmeoSpring therapy uses a computer-enhanced device called an ArmeoSpring—in combination with traditional therapy techniques—to build strength and improve range of motion of a patient’s arm and hand. The ArmeoSpring uses a gravity-assisted exoskeleton to support the arm as the patient interacts with virtual-reality games on a computer screen.
An occupational therapist adjusts the ArmeoSpring exoskeleton to fit the patient’s arm and abilities. Providing support from the shoulder to the hand, the ArmeoSpring counterbalances the weight of the patient’s arm. That can make movement and neuromuscular control easier. In addition, the ArmeoSpring’s computer games motivate patients to participate in their therapy exercises.
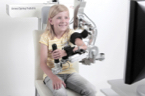
Picture: Hocoma, Switzerland
The ArmeoSpring measures how the arm moves and how the hand grasps. It also detects and assesses a patient’s motor ability, coordination and performance. Our therapists use this information to track progress and decide how difficult the patient’s next exercises should be.
ArmeoSpring therapy gives patients opportunities to work on a variety of hand and arm motions, including:
- Grasp and release.
- Pronation and supination (turning the palm up and down).
- Wrist flexion and extension.
- Shoulder flexion (raising the arm up).
- Shoulder abduction (raising the arm out to the side).
- Shoulder horizontal abduction/adduction (moving the arm across the body).
To help set goals, the occupational therapist asks about the kinds of improvements that would help the patient participate in favorite everyday activities.
Who Can Use ArmeoSpring Therapy?
ArmeoSpring therapy is especially well-suited to patients who have the potential to regain movement or function in their affected arm(s) and hand(s).
ArmeoSpring equipment usually is a good fit for children with arm measurements in the following ranges:
- Forearm length: 9 to 14.5 inches.
- Upper arm length: 6 to 9.5 inches.
Children with arm measurements in those ranges usually are between ages 4 and 15.
Generally, it’s recommended that patients have some ability to move their affected arm when not working against gravity. (For example, while lying on their side or back.)
ArmeoSpring therapy can be appropriate for children even if the affected arm has minimal strength. Even if there’s only movement in one joint (a shoulder, for example), it’s possible to find a virtual exercise appropriate for the patient.
Candidates for ArmeoSpring therapy usually:
- Can follow simple commands.
- Have the visual skills to see a computer screen positioned 2 feet away.
- Can signal or communicate pain, fear or discomfort.
- Understand cause and effect.
- Are medically stable.
- Can tolerate at least 20 minutes of therapy exercise.
- Can complete a program lasting six to nine weeks, without missing appointments.
Gillette provides ArmeoSpring therapy at our St. Paul Campus. Typical sessions last 60 minutes, including 20 to 30 minutes using the ArmeoSpring, followed by other therapy activities addressing functional goals. We also give recommendations for therapy exercises the patient can do at home.
A patient’s care plan might also include additional appointments for assessments. These sessions might not include use of the ArmeoSpring, but they’re important in helping us understand how the therapy program is working for the patient.
At any point during the care plan, the occupational therapist may recommend that the patient child stop ArmeoSpring therapy if the treatment does not appear to be beneficial.
How Do I Get Started With ArmeoSpring Therapy?
To participate in occupational therapy, a doctor’s order is required.
Be sure to check with your insurance company to make sure that your plan covers occupational therapy at the intensive frequency recommended for ArmeoSpring therapy.
How Do I Schedule ArmeoSpring Therapy?
We have two options for scheduling ArmeoSpring therapy:
- Three times per week (Monday, Wednesday and Friday) for six weeks.
- Twice per week (Tuesday and Thursday) for nine weeks.
We schedule additional appointments for an evaluation, an ArmeoSpring fitting, and a follow-up visit.
We have a limited number of schedule timeslots available for ArmeoSpring therapy. If we don’t have a timeslot available when you first request it, we’ll put you on a waiting list.
Your ArmeoSpring Appointments
Plan to arrive 15 minutes early so we can start therapy immediately at the beginning of your appointment.
Bring any braces or splints the patient typically wears on the wrist or hand.
Your child might be tired and have sore muscles or joints. Tell your child’s occupational therapist if these problems last for more than a few hours or interfere with participation in normal activities.
This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.
If you are a Gillette patient with urgent questions or concerns, please contact the Nurse Help Line at 651-229-3890.
 Home Page
Home Page
