What Is A Gastrojejunostomy (GJ) Conversion?
A Gastrojejunostomy (GJ) conversion is converting, or changing, a G-tube to a GJ-tube. Your child will have a tube that goes directly into the stomach (via G-tube) and one that goes past the stomach into the Jejunum (J-tube).
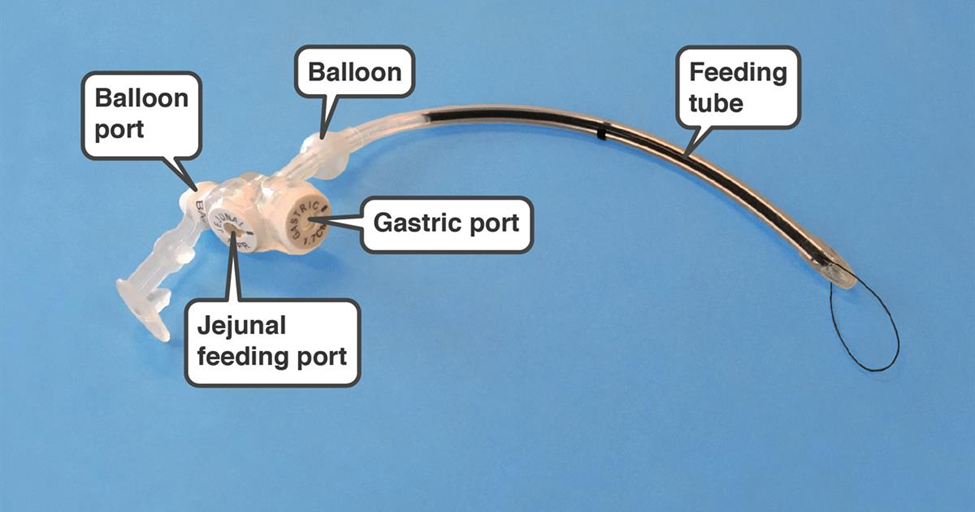
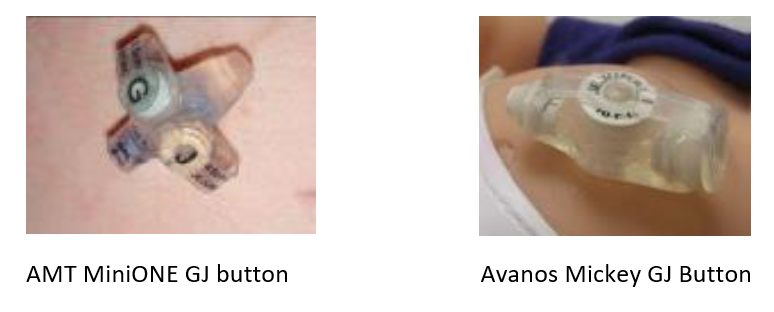
Who Benefits From A GJ Conversion?
Surgical patients may have their G-tube converted to a GJ-tube to help with post-operative recovery. A patient’s G-tube may also be converted to GJ-tube to improve feeding tolerance.
Preparing For GJ Conversion
NPO (nothing by g-tube or by mouth) is allowed 3 hours prior to the procedure. Please follow any other specific guidelines given by your child's provider.
What To Expect With A GJ Conversion
- The G-tube is converted to a GJ-tube in Interventional Radiology. If done for surgery, this is usually done a week or so prior to surgery.
- If done for surgery, feedings should be done through the G-Port, per normal routine. If done for other reasons, please discuss with the ordering provider for a feeding plan.
- Site care should be done per normal routine.
- DO NOT twist or rotate the GJ-tube as this will create a “corkscrew effect”.
- The Jejunal port should be flushed with a small amount of water, 10-20ml, twice daily. Use warm tap water and push slowly to prevent cramping. Do not force this, if you are unable to flush, stop and call the Gillette Nurse Help Line.
- GJ-tube exchanges will be needed if this is a more permanent conversion to a GJ-tube. It is recommended that it be changed every 4-6 months or sooner if needed. This may be done in the operating room by a surgeon or in Interventional Radiology. Conversion to a gastrostomy tube (stomach only) may be done in clinic. Please schedule as directed by your child's provider.
- If symptoms of migration, call the Gillette Nurse Help Line and they can devise a plan. Symptoms include feeding intolerance, fullness and/or discomfort. An ER or hospital visit may be necessary to see if the tube migrated back to the stomach.
- In case of tube dislodgement, call the Gillette Nurse Help Line or your child's provider for next steps.
What To Expect If The GJ conversion Was Done For Surgery
Post-op feeding will start through the Jejunal port (J port), which allows feeding to resume sooner and can avoid reflux from the stomach. Feedings will be advanced during your child's hospital stay with the goal of converting back to G-tube feedings, per normal routine. The GJ-tube will be changed back to a G-tube once this has been done. Sometimes, patients are sent home with a GJ-tube, if needed, to get back to baseline feeding. These instructions will be provided to you at time of discharge with a follow-up plan in place.
If symptoms of migration, call the Gillette Nurse Help Line and they can devise a plan. Symptoms include feeding intolerance, fullness and/or discomfort. An ER or hospital visit may be necessary to see if the tube migrated back to the stomach so that they can do imaging/x-ray to confirm placement.
This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.If you are a Gillette patient with urgent questions or concerns, please contact the Gillette Nurse Help Line at 651-229-3890.
Translations
This information is for educational purposes only. It is not intended to replace the advice of your health care providers. If you have any questions, talk with your doctor or others on your health care team.
If you are a Gillette patient with urgent questions or concerns, please contact the Nurse Help Line at 651-229-3890.
 Home Page
Home Page
