What is Vertebral Body Tethering (VBT)?
Vertebral Body Tethering (VBT) is a scoliosis surgery used to treat scoliosis. Gillette Children’s offers several options for scoliosis treatment including VBT, which uses the body’s growth to correct spine curvature without the need for spinal fusion.
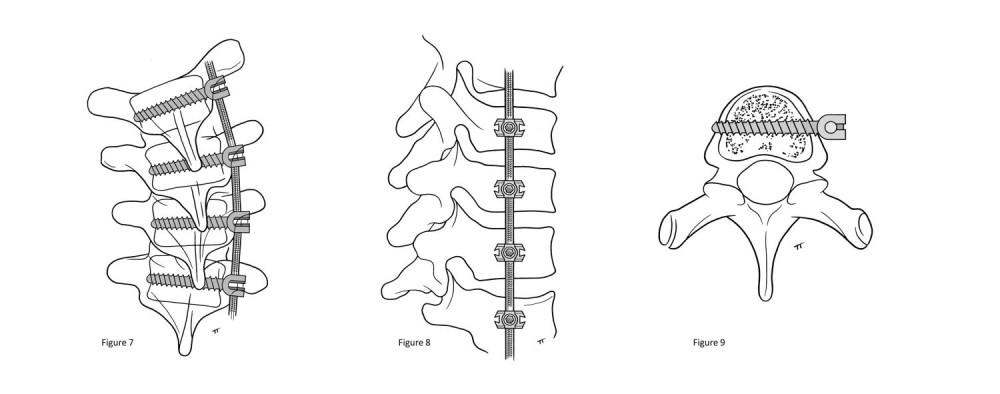
In Vertebral Body Tethering (VBT) surgery, a spine surgeon and general surgeon work together to place screws in the vertebrae on the convexity (outside) of the curve and connect the screws with a strong rope called a tether. The tether is tensioned to slow down growth on the outside part of the curve while allowing for continued growth on the concavity (inside) of the curve. As such, the body’s natural growth allows for curve correction over time. The surgical procedure lasts approximately 4 hours and the expected length of hospital stay is 2-3 days.
The surgery can help to:
- Straighten a crooked spine or spine curvature.
- Improve sitting and balance.
Who can get VBT surgery?
Because the success of the procedure relies on the spine continuing to grow, patients need to meet very specific criteria to be a candidate for this surgery. At Gillette, our typical criteria for performing a VBT surgery include:
- A spinal curve with Cobb measurement of 40 degrees to 65 degrees
- A spinal curve that is flexible and reduces to 35 degrees and lower on bending films
- A candidate whose spine will continue to grow (typically assessed with a hand x-ray)
Several risk factors may impact VBT surgery eligibility. Your Gillette provider will discuss any of these risks with you.
The theoretical* advantages of VBT are preserved spinal motion and growth, which has the benefit of improved spinal flexibility and reduced stress on other areas of the spine. By decreasing the amount of stress the spine withstands over time, degenerative (age-associated) changes may be less likely.
Additionally, VBT is often performed in a “minimally-invasive” fashion through small incisions in the side of the chest or abdomen with the assistance of a fiber-optic video camera. The minimally-invasive nature of the procedure is associated with decreased blood loss and faster recovery time when compared to traditional spinal fusion.
*It is important to note that long-term results for vertebral body tethering are unknown. The overall rate of “success” (defined as reaching skeletal maturity with a spinal curve <35 degrees) is between 70%-75%.
COMPARISON TABLE PSF vs. VBT
| Spine Fusion | Vertebral Body Tethering |
|---|---|
| Reliable curve correction and long term maintenance of that correction | Common to have a residual curve, long term outcomes unknown |
| Reoperation rate 10-15% | Reoperation rate 20-40% |
| Able to correct the curvature and rotation- straighter spine and decreased rib prominence | Able to correct curvature only- straighter spine, but rib prominence often remains unchanged |
| Very small but real risk of neurological injury- paralysis, loss of sensation, nerve damage | Very small, but real risk of neurological injury- paralysis, loss of sensation, nerve damage |
| More control over upper portion of spine in order to achieve shoulder balance | Can cause worsening or change in shoulder height imbalance |
| Decrease in flexibility and range of motion | Retained flexibility and range of motion |
| Overcorrection is not a risk | Overcorrection of curve following the procedure is a risk |
| Increase stress on the vertebra and discs above and below level of fusion with potential for increased risk of disc degeneration in unfused segments later in life | Possibly less stress over time, less disc degeneration later in life |
| All curves in the thoracic and lumbar regions can be corrected | Upper thoracic spine (above T4) is not able to be corrected |
How does VBT surgery compare to spine fusion surgery?
You can help make sure your child has the best possible outcome by understanding what to expect before, during and after spinal fusion surgery at Gillette Children’s. Here are a few resources to help you feel more prepared:
- Review tips to prepare for surgery at Gillette.
- Understand the amenities available at Gillette.
We offer a tour of Gillette before surgery for our patients and their families. This is not only a tour of the building; our child life team will discuss various coping mechanisms and resources available to make your stay as comfortable as possible. They will also assess what the patient and family may be most anxious about regarding their surgery and hospital stay, and use various techniques to lessen this anxiety as much as possible. We recommend this visit within 2-3 weeks before surgery.
Your care team at Gillette will reach out to you to:
- Obtain a health history, including details about medicines (name, dose and frequency), pharmacy and primary care doctor.
- Discuss what to expect on the day of surgery and during the hospital stay.
Let you know what you’ll need when you leave the hospital.
Overall health can affect how well and how quickly your child recovers from spinal fusion surgery. Your child should maintain regular levels of activity and physical therapy before surgery. Eating adequate amounts of food with iron, calcium, and vitamins C and D (fresh colorful fruits and vegetables, dairy food, and other products with added iron and calcium) is helpful, too.
Gillette is a latex-free facility, but it’s still important to tell us if your child has a latex allergy or has ever had a severe reaction to latex.
Sometimes fears, behavior or expectations related to the upcoming surgery cause stress for families. Contact your child’s primary health care provider or Child and Family Services for support. Gillette can help with resources that might help reduce anxiety for all of your family members. Our child life specialists can provide emotional support and distractions (such as toys and movies we can bring to the preoperative waiting area before surgery begins). Child life specialists also can meet with your child’s siblings to address their feelings and concerns.
Knowing what to expect can help everyone feel more prepared. We’ll be sure to help clarify short- and long-term expectations for outcomes following VBT surgery.
 Home Page
Home Page
